Best Hospital in Ghatkopar, Mumbai | Zynova Shalby Hospital
Blogs Zynova
- admin
- 0 Comments
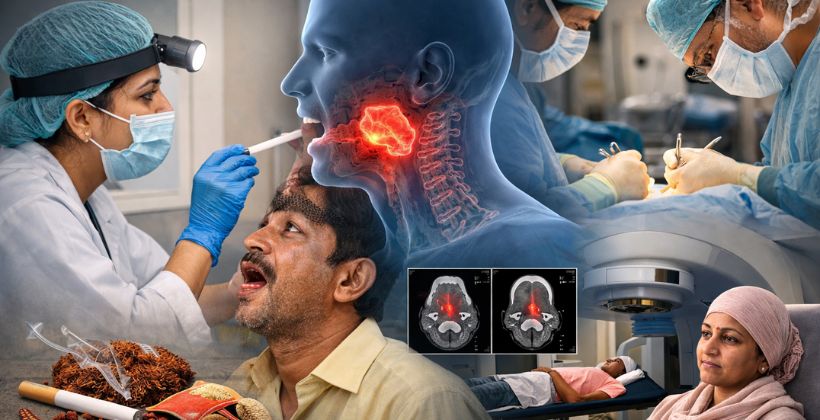
Head and Neck Cancer in India: Causes, Early Warning Signs, Diagnosis and Treatment Options Explained by Expert Oncologists in Mumbai
Introduction: A Cancer That Touches Too Many Families in India Imagine this. A 48-year-old man from Ghatkopar visits a dentist because of a mouth sore that has been bothering him for about six weeks. He assumes it is from the hot chai he drinks every morning. The dentist takes one look and immediately refers him to an oncologist. Within days, he is diagnosed with Stage 2 oral cancer. The good news? He caught it at a stage where surgery alone could treat him. He is now two years cancer-free. This story is real. And it happens far too rarely in India, because most people wait months, sometimes even years, before seeking medical help for symptoms that could be early warning signs of head and neck cancer. Head and neck cancer is not a rare disease in our country. India carries one of the highest burdens of this cancer in the entire world. According to data from the National Cancer Registry Programme of India, head and neck cancers collectively make up nearly 25 to 30 percent of all new cancer cases diagnosed each year. That is hundreds of thousands of patients annually. And yet, awareness remains surprisingly low. This blog is written for you: the patient who is searching for answers, the family member sitting beside someone who has just been diagnosed, and the person who has been ignoring a symptom for too long. We will walk you through everything, from what this cancer is, what causes it, what the warning signs look like, how it is diagnosed, and what modern head and neck cancer treatment Mumbai options are available today. We will also explain when it is time to stop googling and start talking to a best oncologist in Mumbai or an oncologist near me Ghatkopar. What Is Head and Neck Cancer? Head and neck cancer is an umbrella term used for cancers that start in the structures of the head and neck region. This is not one single cancer but rather a family of different cancers, each with its own behavior, treatment, and prognosis. Understanding these subtypes is essential whether you are searching for a head neck cancer specialist in Ghatkopar or consulting the best cancer hospital in Mumbai. The most common sites include: Oral cavity: The lips, tongue, gums, inner cheeks, floor of the mouth, and the hard palate (roof of the mouth). Oral cancer is the most common type seen in India. Oropharynx: The middle part of the throat, including the soft palate, the back of the tongue, the tonsils, and the back wall of the throat. HPV-related throat cancers often arise here. Hypopharynx: The lower part of the throat, just above the food pipe (esophagus). Cancers here are often detected late because symptoms are subtle. Larynx (voice box): Cancers here often present with voice changes. Smokers are particularly at risk. Nasopharynx: The upper part of the throat behind the nose. This type is more common in people of Southeast Asian origin. Nasal cavity and paranasal sinuses: Cancers in these air-filled spaces behind the nose and cheeks. Salivary glands: The parotid, submandibular, and smaller salivary glands can develop tumors, some benign and some malignant. Thyroid gland: Though often discussed separately, thyroid cancers are anatomically part of head and neck oncology. Most head and neck cancers are squamous cell carcinomas, meaning they arise from the flat squamous cells that line the inner surfaces of these organs. However, adenocarcinomas, mucoepidermoid carcinomas, and other rarer types also occur. A head neck cancer doctor in Mumbai or a surgical oncologist in Mumbai with specialized training can identify the specific subtype through biopsy and guide treatment accordingly. How Common Is Head and Neck Cancer in India? India has a disproportionately high burden of head and neck cancers compared to most other countries. Here are some facts that put this into perspective: Oral cancer alone accounts for nearly 11 percent of all cancers in Indian men and is one of the most common cancers in the country. India has among the highest rates of oral and pharyngeal cancers in the world, largely driven by tobacco and betel nut use. Approximately 77,000 new cases of oral cancer are diagnosed in India every year, according to estimates from the Indian Council of Medical Research. In Maharashtra, and particularly in Mumbai, the combination of tobacco chewing habits, alcohol consumption, and lifestyle factors makes head and neck cancers a significant public health concern. More than 70 percent of patients in India present at an advanced stage (Stage 3 or Stage 4), which makes treatment more complex and outcomes less favorable. These numbers are sobering, but they also point to a clear opportunity: better awareness leads to earlier diagnosis, which leads to better survival. That is exactly why this information matters. Head and Neck Cancer Causes: What Puts You at Risk? Understanding what causes or contributes to head and neck cancer can help individuals take preventive action and recognize when they might be at higher risk. The causes are a mix of lifestyle habits, infections, environmental exposures, and sometimes just biology. Tobacco: The Single Biggest Risk Factor in India There is no getting around this. Tobacco in all its forms is responsible for the majority of head and neck cancers in our country. The risk applies to: Cigarette smoking Bidi smoking (which is more common in rural and semi-urban India and delivers higher concentrations of carcinogens) Hookah or sheesha smoking Chewing tobacco, gutka, mawa, khaini, and paan masala Betel nut (supari) chewing, often combined with lime and tobacco The tobacco cancer risk in India is significantly amplified because smokeless tobacco use is deeply normalized in many communities. People do not see chewing gutka as dangerous because it does not produce smoke. But the carcinogens in smokeless tobacco directly contact the lining of the mouth, causing cellular damage that, over years, can turn into cancer. Chewing tobacco also leads to a condition called oral submucous fibrosis (OSMF), where the tissues of the mouth gradually harden and restrict mouth
- admin
- 0 Comments
10 Health Problems Mumbai’s Summer Heat Causes and How Zynova Shalby Hospital Treats Each One
Mumbai in summer is not just uncomfortable. It is genuinely dangerous. By April, the city pushes past 38-40 degrees Celsius. Add Mumbai’s notorious humidity on top of that, and the body works twice as hard just to stay cool. By April and May, emergency rooms start filling up. At Zynova Shalby Hospital, Ghatkopar, our doctors see it every year. Patients who waited too long. People who mistook a warning sign for plain tiredness. Families who did not realize that what their loved one was experiencing was a medical emergency. This blog covers the 10 most common health problems Mumbai’s summer heat causes. For each one, you will find the warning signs, who is at risk, what to do at home, and how our multispecialty team at Zynova Shalby Hospital treats it. Whether you live in Ghatkopar, Vikhroli, Kanjurmarg, Mulund, Bhandup, Kurla, or anywhere in the eastern suburbs, save this as your summer health reference. Why Mumbai’s Summer Heat Is Medically Different From the Rest of India Most heat-related health guides are written for dry heat conditions. Delhi, Rajasthan, and central India face brutal dry heat. Mumbai’s summer is a different problem entirely. The combination of high temperature and high humidity makes Mumbai’s summer uniquely dangerous from a medical standpoint. When the air is already saturated with moisture, sweat cannot evaporate from the skin efficiently. Sweating is the body’s primary cooling mechanism. When that system cannot work properly, body temperature rises faster and stays elevated longer. The risk of heat stroke, dehydration, electrolyte imbalance, and kidney stress is significantly higher in humid heat than in dry heat of the same temperature. This is why Mumbai sees spikes in heat-related hospital admissions even at temperatures that might seem manageable in other parts of the country. Construction workers, auto-rickshaw drivers, street vendors, delivery riders, domestic workers, and daily wage laborers bear the highest risk because they cannot avoid outdoor exposure during peak hours. But office-goers commuting on crowded trains, school children, and senior citizens at home in poorly ventilated rooms are also at real risk. Heat Stroke Symptoms, Causes, and Emergency Treatment in Mumbai What Is Heat Stroke Heat stroke is the most dangerous heat-related illness and is a full medical emergency. It happens when the body’s core temperature rises above 40 degrees Celsius (104°F) and the natural cooling system stops working entirely. Without treatment, heat stroke can cause permanent damage to the brain, heart, kidneys, liver, and muscles within minutes. Every minute of delay increases the risk of death or permanent injury. Heat deaths across India exceed fatalities from floods, cyclones, and earthquakes combined each year. In a dense, humid city like Mumbai, the risk is real for everyone. Two Types of Heat Stroke Classic Heat Stroke develops over one to two days of prolonged heat exposure. It does not require physical exertion. Elderly people, infants, and those with chronic illnesses like diabetes, heart disease, or hypertension are most vulnerable. An older person sitting in a hot, poorly ventilated room for two days during a Mumbai heatwave can develop classic heat stroke without ever stepping outside. Exertional Heat Stroke develops fast, sometimes within an hour of heavy physical activity in the heat. Construction workers, delivery riders, athletes, and outdoor laborers in Mumbai are at highest risk. It can develop during morning shifts before the body has fully adjusted to the heat. Heat Stroke Symptoms to Watch For Knowing the heat stroke symptoms can save a life because this condition moves fast. Early warning signs: Throbbing headache Dizziness and light-headedness Lack of sweating despite the heat (this is a red flag, not relief) Red, hot, dry skin Muscle weakness or cramps Nausea and vomiting Rapid, strong heartbeat Advanced heat stroke symptoms that require immediate emergency care: Body temperature above 40°C (104°F) Confusion, disorientation, or slurred speech Loss of consciousness or seizures Rapid, shallow breathing Extreme agitation or strange behavior that is out of character One sign many people miss: when someone suddenly stops sweating in intense heat, that is not relief. That means the cooling system has completely failed. Call for help immediately. Heat Exhaustion vs Heat Stroke: Understanding the Difference This is one of the most important distinctions in summer emergency medicine. Heat exhaustion is the body’s warning before it crosses into emergency territory. Signs include heavy sweating, cold clammy skin, a fast but weak pulse, nausea, muscle cramps, weakness, and feeling faint. The person is still conscious and can respond to questions normally. Heat exhaustion can usually be managed by moving to a cool space, drinking ORS or electrolyte fluids, and applying cool compresses to the skin. Heat stroke is the emergency. The key differences are: skin is hot and dry rather than cold and clammy, body temperature is above 40°C, and the person shows confusion, disorientation, or loss of consciousness. Heat stroke requires immediate emergency medical treatment. Do not try to manage it at home. If you are unsure which situation you are dealing with, treat it as heat stroke and get to a heat stroke emergency hospital in Mumbai right away. Heat Stroke First Aid India: What to Do Before Help Arrives These steps can be the difference between full recovery and permanent injury. Step 1: Move the person out of the sun immediately. Get them indoors or into shade. Step 2: Call for emergency transport to the nearest heat stroke emergency hospital in Mumbai. At Zynova Shalby Hospital in Ghatkopar, our emergency line is available 24 hours. Step 3: Remove excess clothing to expose more skin surface for cooling. Step 4: Apply ice packs or cold wet cloths directly to the neck, armpits, and groin. These are the areas where large blood vessels run close to the skin, so cooling here brings body temperature down fastest. Step 5: Fan the person continuously while pouring cool water over the skin. This mimics the evaporative cooling that sweating normally provides. Step 6: If the person is conscious and able to swallow without difficulty, give small sips of cool water
- admin
- 0 Comments
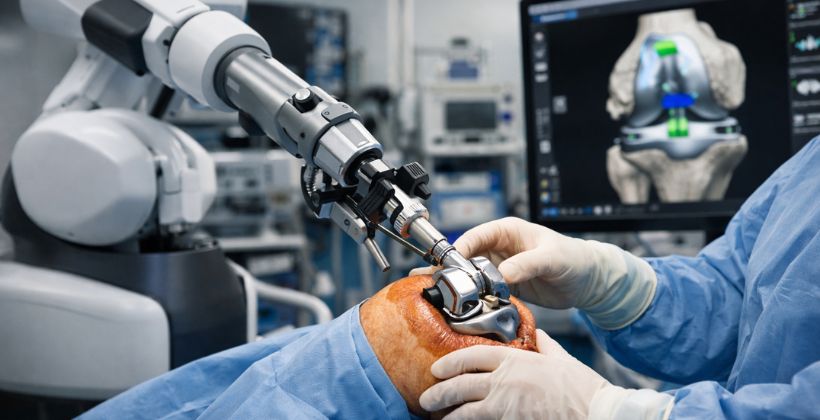
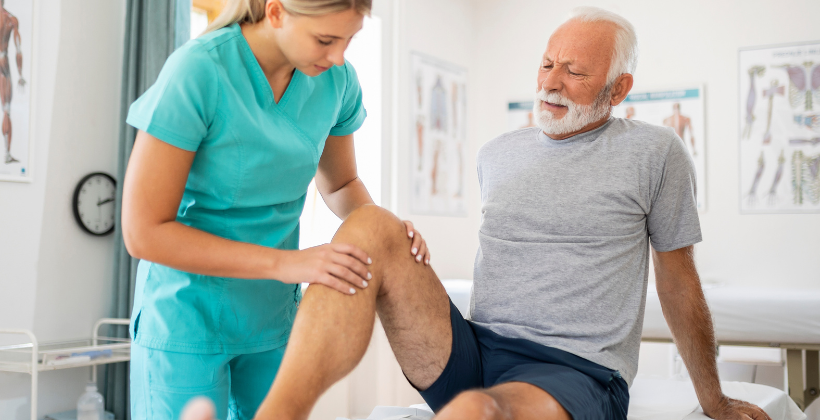
Robotic Joint Replacement Surgery: A New Era in Knee and Hip Replacement
Your Knee Pain Is Telling You Something. Are You Listening? Most people ignore knee pain at first. It starts as a mild ache after a walk, a little stiffness in the morning, or an odd sound when going up the stairs. Easy to brush off. But over time, that quiet discomfort turns into something that stops you from doing the things you love. If your knee pain has reached a point where daily life is getting harder, you may be among the many patients who need robotic knee replacement surgery. And the earlier you pay attention to the warning signs, the better your chances of getting back to a pain-free, active life. At Zynova Hospitals, we use advanced robotic knee surgery technology that is built to handle more than just the knee. Our robotic system performs robotic total knee replacement, robotic partial knee replacement, and robotic hip replacement, all with the same level of precision and care under one roof. This blog walks you through the early warning signs of knee joint damage and helps you understand when it is time to consider robotic knee replacement surgery for lasting relief. What Actually Happens to Your Knee When It Gets Damaged? The knee is the largest joint in your body. It carries your full body weight with every step, squat, and climb. The cartilage inside the knee acts as a cushion between the bones, keeping movement smooth and pain-free. When that cartilage starts breaking down, the bones begin rubbing against each other. That is when the pain, swelling, and stiffness start. The most common reasons this happens are: Osteoarthritis: The most common cause of knee damage. Cartilage slowly wears away over the years, mostly in people above 50. But younger people with a history of injury or high-impact sports can develop it early too. Rheumatoid Arthritis: An autoimmune condition where the body’s immune system attacks the joint lining itself, causing chronic swelling, cartilage damage, and bone loss. Post-Traumatic Arthritis: This develops after a knee fracture, ligament tear, or sports injury. Sometimes it shows up years after the original injury. Avascular Necrosis: When blood supply to the knee bone gets cut off, the bone tissue dies and the joint collapses from the inside. In all of these cases, once the damage goes past a certain point, robotic total knee replacement becomes the most reliable long-term solution. 7 Signs You May Need Robotic Knee Replacement Surgery Not every sore knee needs surgery. But there are clear signs that your joint damage has gone far enough that non-surgical options are no longer doing the job. Here are the seven signs that should push you to speak to an orthopedic specialist: 1. The Pain Does Not Go Away Even When You Rest In the early stages, knee pain usually shows up after physical activity and settles once you rest. But when the pain sticks around even when you are sitting, lying down, or sleeping, it means the damage has gone deeper. At this stage, painkillers and anti-inflammatory medicines stop giving proper relief. This kind of persistent pain is one of the key signs you need knee replacement surgery. 2. Your Knee Swells Up and Stays Swollen A little swelling after a long day is normal. But if your knee stays puffy for days at a time or swells back up quickly after settling, that is not normal. Chronic swelling means the inside of your joint is badly damaged and cannot heal on its own. This is one of the clearest early signs that you should get evaluated for robotic knee surgery. 3. You Cannot Straighten or Bend Your Knee Properly When the knee joint is healthy, it bends and straightens without any trouble. As cartilage damage gets worse, the joint loses its range of motion. You may find it hard to fully straighten your leg, bend your knee to sit, climb stairs, or stand up from a chair. When basic movements start becoming difficult, it is time to take the warning seriously. 4. You Hear Grinding or Clicking or Feel the Knee Lock Up A healthy knee is quiet and smooth. When the cartilage wears away, the bone surfaces grind against each other. You may notice: A crunching or grating sensation when you move the knee (called crepitus) Clicking or popping sounds with movement The knee suddenly locking or getting stuck for a moment These are mechanical signs of serious cartilage loss. They are also important clinical indicators that an orthopedic specialist will look for when assessing a patient for advanced robotic knee surgery. 5. Your Knee Looks Different or Bent Out of Shape As arthritis gets worse, the structure of the knee can change visibly. Some patients develop a bow-legged look (varus deformity), while others develop a knock-knee shape (valgus deformity). In some cases, one leg may appear shorter than the other. Visible deformity is a strong indicator that surgery is required. Robotic total knee replacement is especially useful in these situations because the robotic arm uses real-time 3D imaging to correct alignment with sub-millimetre precision, even in complex cases. 6. Knee Pain Is Stopping You from Living Your Life When knee pain starts cutting into your daily routine, that is when it becomes a real problem. Ask yourself honestly: Have you stopped doing activities or hobbies you used to enjoy? Do you need a cane or support to walk? Is knee pain waking you up at night? Can you not walk or stand for more than 20 to 30 minutes? If you said yes to most of these, your condition has gone far enough that robotic knee replacement surgery deserves a serious conversation with a specialist. 7. Nothing Else Is Giving You Relief Anymore Doctors always try non-surgical options first. These include: Physiotherapy and muscle-strengthening exercises Anti-inflammatory medicines and painkillers Steroid injections or PRP (platelet-rich plasma) therapy Weight management and activity changes Knee braces and orthotics If you have gone through these treatments properly and are still in pain, you have crossed
- admin
- 0 Comments
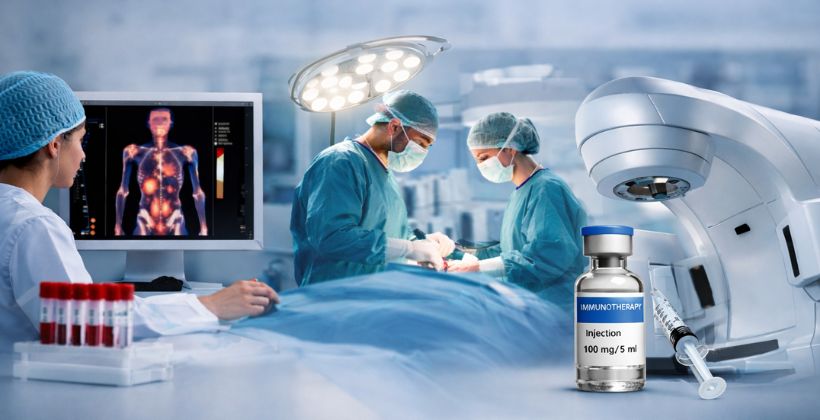
Advanced Cancer Treatment in Mumbai: Choosing the Best Hospital for Quality Care
Getting a cancer diagnosis is not something anyone is prepared for. The moment that word is spoken, everything else fades into the background. Fear, confusion, and hundreds of questions come rushing in at once. Where do I go? Who do I trust? Will I get the right care? If you are in Mumbai and you are asking these questions right now, this blog is written for you. Mumbai has some of the strongest cancer care in the country. The doctors are skilled, the hospitals are well-equipped, and access to advanced cancer treatment is genuinely available here. But knowing where to go and what to look for still makes a real difference – because not all cancer hospitals in Mumbai are built the same way. This guide walks you through everything you need to know – the treatment options available today, what to look for in a good cancer hospital in Mumbai, and why Zynova Hospitals Pvt. Ltd. in Ghatkopar is the name more and more patients across Mumbai are coming to rely on. Cancer Care in Mumbai Has Come a Long Way It was not long ago that a cancer patient in Mumbai had very limited choices. Treatment was largely concentrated in a handful of hospitals; waiting times were long, and for patients living in the eastern or central parts of the city, getting quality oncology care meant long hours of travel for every appointment, every chemotherapy session, and every follow-up. Things are very different now. The rise of dedicated oncology hospitals in Mumbai has changed the landscape entirely. Patients living in areas like Ghatkopar, Vikhroli, Kurla, Mulund, and Chembur now have access to serious, specialized cancer care without having to travel to the far ends of the city. And the level of treatment available at these hospitals in terms of technology, expertise, and the range of options offered is genuinely world-class. Zynova Hospitals Pvt. Ltd. on LBS Marg, Ghatkopar West, is one of the strongest examples of this shift. As a cancer treatment hospital in Mumbai that brings surgical, medical, and radiation oncology together under one roof, it gives patients access to a full range of advanced cancer treatment in Ghatkopar – a part of the city that needed exactly this kind of dedicated oncology care. What Advanced Cancer Treatment Actually Looks Like Today People often hear the phrase ‘advanced cancer treatment‘ and assume it means something complicated or experimental. In reality, it simply means that your treatment is built specifically around your cancer – its type, its stage, its genetic make-up – and that your doctors have access to the latest tools and methods to treat it. Here is what that looks like in practice at a good oncology hospital in Mumbai today. Chemotherapy, Targeted Therapy and Immunotherapy Medical oncology covers the medicine-based side of cancer treatment. For years, chemotherapy was the main weapon – drugs that kill fast-growing cancer cells throughout the body. Chemotherapy is still widely used and extremely effective for many cancer types, and a well-run chemotherapy hospital in Mumbai will administer it in a way that is carefully dosed and closely monitored. But today, chemotherapy is just one option among several. Targeted therapy uses drugs that are designed to hit specific changes inside cancer cells – meaning the treatment is more precise and often easier on the body than traditional chemo. Immunotherapy works differently again. Instead of directly attacking the cancer, it trains your own immune system to recognise cancer cells and fight them. For many patients, immunotherapy has delivered results that were not possible even a few years ago. The best oncologist in Mumbai for your case is not necessarily the one with the most impressive title – it is the one who looks at your specific cancer and builds a treatment plan that gives you the best possible outcome with the least unnecessary side effects. Cancer Surgery Done Right Surgery is still one of the most effective treatments for many types of cancer, particularly when the tumour is caught early and has not spread. But cancer surgery today looks very different from what it used to be. Minimally invasive techniques, laparoscopic tools, and increasingly, robotic-assisted procedures mean smaller incisions, less blood loss, faster recovery, and less pain. A good cancer surgery team in Mumbai is not just technically skilled – they plan carefully. They consider the tumour’s location, its relationship to surrounding tissue, and the patient’s overall health before deciding on the best surgical approach. The goal is always to remove the cancer while preserving as much of the patient’s quality of life as possible. Radiation Therapy – More Precise Than Ever Radiation therapy has been part of cancer treatment for a long time, but modern radiation is a very different thing from what it was a decade or two ago. Techniques like Intensity Modulated Radiation Therapy – IMRT – allow radiation oncologists to shape the beam to match the exact outline of a tumour, delivering a high dose to the cancer while protecting the healthy tissue around it. Image Guided Radiation Therapy, or IGRT, takes things further by tracking the position of the tumour in real time during treatment, adjusting for any small movements the patient makes. The result is radiation that is more effective and comes with fewer side effects – which matters a great deal for patients who are already managing a physically demanding treatment journey. Care That Looks After the Whole Person This one does not always get talked about enough. Advanced cancer treatment is not only about attacking the tumour. It is also about making sure the person living with cancer is supported – physically, emotionally, and practically. Palliative care, nutritional support, pain management, and psychological counselling are all part of what a truly complete cancer care centre in Mumbai should offer. A patient who is well-nourished, well-rested, and emotionally supported tends to respond better to treatment. That is not a soft addition to cancer care – it is a clinical reality, and the best oncology
- admin
- 0 Comments
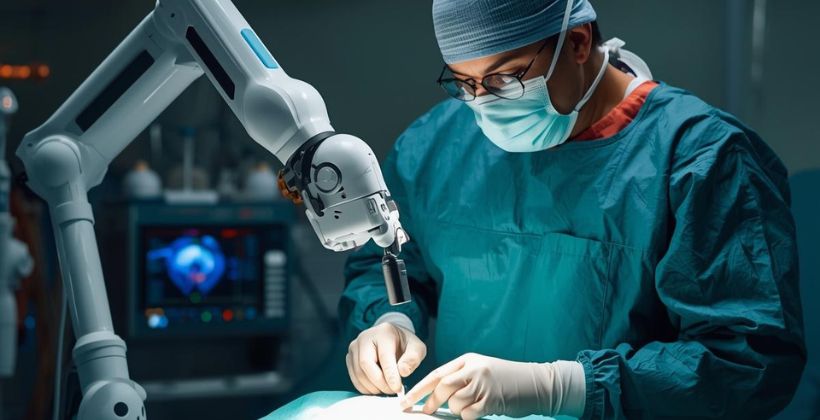
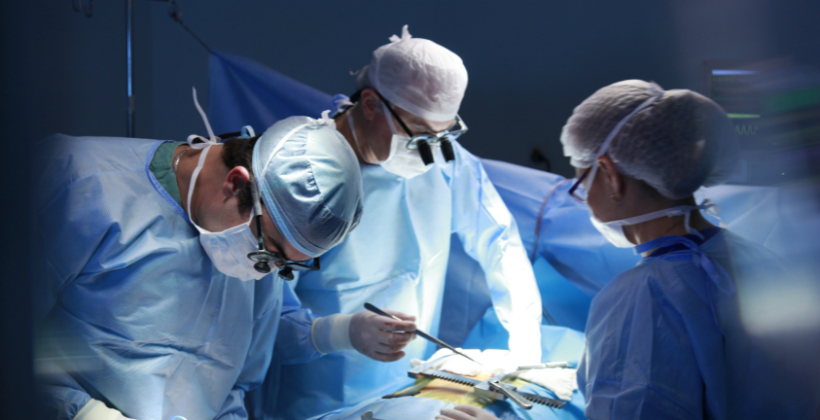
What Is Robotic Surgery? How It Works, Who Is Eligible & Is It Safe?
Understanding Robotic Surgery Robotic surgery, also called robotic assisted surgery, is an advanced surgical technique where doctors use a robotic system to perform complex procedures with high precision and control. Despite the name, the robot does not operate on its own. The surgeon remains fully in control at all times. In simple words, robotic surgery is a modern form of minimally invasive surgery that allows surgeons to operate through small cuts using robotic arms guided by a computer system. Over the last decade, robotic surgery in Mumbai and worldwide has grown rapidly. Patients prefer it because it offers less pain, smaller scars, faster recovery, and better surgical accuracy compared to traditional open surgery. With the growing demand for advanced surgery in India, especially in cities like Mumbai, more hospitals are adopting robotic surgical technology. However, choosing the right hospital and experienced robotic surgeon is extremely important for safety and results. What Is Robotic Surgery? Definition of Robotic-Assisted Surgery Robotic surgery, also known as robotic assisted surgery, is an advanced form of minimally invasive surgery in which a specially trained surgeon uses a robotic system to perform complex surgical procedures with enhanced precision, flexibility, and control. In robotic surgery, small surgical instruments are attached to robotic arms, which are controlled entirely by the surgeon from a computerized console. The system provides high-definition, 3D magnified vision and allows extremely precise movements that are often beyond the capability of the human hand alone. Robotic surgery represents one of the most significant advancements in modern and advanced surgery, improving outcomes across multiple specialties. Does the Robot Operate Independently? No, the robot does not operate independently. One of the most common misconceptions about robotic surgery is that the robot performs the surgery on its own. This is not true. In robotic assisted surgery, the surgeon remains in complete control throughout the procedure. The robotic system does not: Make decisions Move without instruction Replace the surgeon Instead, it translates the surgeon’s hand movements into smaller, more precise movements inside the patient’s body. If the surgeon stops, the robot stops immediately. Difference Between Robotic Surgery and Automated Surgery Robotic surgery is often confused with automated surgery, but they are very different. Automated surgery: Machines function independently using programmed instructions. Robotic assisted surgery: The surgeon controls every action in real time. Robotic surgery enhances human skill — it does not replace human expertise. The technology serves as an extension of the surgeon’s hands, eyes, and precision. Role of the Surgeon in Robotic Procedures During robotic surgery, the surgeon: Sits at an advanced control console Views a magnified 3D HD image of the surgical area Controls robotic arms using hand and foot controls Performs delicate surgical steps with high precision The robotic system filters out natural hand tremors and enhances fine movements. However, every movement originates from the surgeon. This combination of human expertise and robotic precision improves surgical accuracy, reduces complications, and enhances patient outcomes. Evolution of Robotic Surgery Surgery has evolved dramatically over the past century. 1. Open Surgery Traditional open surgery required large incisions. Although effective, it involved: More blood loss Higher infection risk Longer hospital stays Slower recovery 2. Laparoscopic Surgery Laparoscopic (keyhole) surgery introduced smaller incisions and camera guidance. It reduced recovery time but had limitations such as: Limited range of motion 2D visualization Restricted instrument movement 3. Robotic Surgery Technology Robotic surgery was developed to overcome these limitations. It offers: 3D high-definition vision Greater instrument flexibility Enhanced dexterity Improved precision Today, robotic surgery in India is expanding rapidly across orthopaedics, urology, gynaecology, and oncology. Globally, robotic assisted surgery is becoming the preferred option for many complex and minimally invasive procedures. How Does Robotic Surgery Work? (Step-by-Step) Understanding how robotic surgery works helps patients feel informed and confident. 1. Pre-Operative Planning Before surgery, doctors conduct: Blood investigations CT scans or MRI Detailed imaging studies Physical examination These tests help create a precise surgical plan tailored to the patient. 2. Anaesthesia The patient is given general anaesthesia so they remain asleep and pain-free during the procedure. 3. Small Incisions Instead of a large cut, the surgeon makes small incisions (usually 1–2 cm). 4. Insertion of Robotic Arms Robotic arms equipped with tiny surgical instruments are inserted through these small cuts. 5. 3D HD Camera Vision A high-definition camera provides a magnified 3D view, sometimes up to 10 times magnification. This allows the surgeon to see delicate structures clearly. 6. Surgeon-Controlled Movements The surgeon controls the robotic arms from a console. The system translates large hand movements into micro-movements inside the body, ensuring: Higher precision Better stability Minimal tissue damage Reduced bleeding What Does the Robot Actually Do During Surgery? The robotic system enhances surgical performance by: Improving precision and control Filtering out hand tremors Allowing 360-degree wrist rotation Operating in tight and hard-to-reach areas Increasing surgical consistency It does not replace the surgeon. Instead, it acts as a highly advanced surgical assistant. Types of Surgeries Performed Using Robotic Technology Robotic surgery applications are growing rapidly in India and worldwide. 1. Orthopaedic Robotic Surgery Robotic hip replacement surgery Robotic knee replacement Robotic spine surgery Robotics helps ensure accurate implant positioning and joint alignment. 2. Gynaecology Robotic Surgery Robotic hysterectomy Fibroid removal Endometriosis surgery 3. Urology Robotic Surgery Robotic prostate surgery Kidney tumor removal Bladder reconstruction 4. Cancer and General Surgery Colorectal cancer surgery Gastrointestinal surgery Lung surgery Robotic surgery in cancer care improves tumor removal precision while preserving healthy tissue. Who Is Eligible for Robotic Surgery? Robotic surgery eligibility depends on multiple factors. Ideal Candidates: Patients requiring minimally invasive procedures Early-stage cancer patients Joint replacement patients Patients seeking faster recovery Factors Doctors Evaluate: Age Overall health condition Disease stage Complexity of surger Previous surgical history A detailed medical evaluation determines whether robotic assisted surgery is suitable. Who May Not Be Suitable for Robotic Surgery? Certain patients may not be ideal candidates: Emergency surgical cases Severe heart or lung disease Extremely advanced disease High surgical risk patients Final decision is always made after thorough consultation with
- admin
- 0 Comments
Comprehensive Oncology Care: Diagnosis, Treatment & Follow-Up Under One Roof
Why Comprehensive Oncology Care Is the Need of Today Cancer is no longer a rare disease. In the global community, and especially in India, the incidence of cancer is rising at an alarming rate due to lifestyle changes, pollution, the use of tobacco products, and the aging population. Now it is one of the most common causes of deaths worldwide. With modern medical advancements, early detection and timely treatment can significantly improve survival. However, patients can benefit from these advances only when they have access to comprehensive oncology care. Many patients face challenges because cancer treatment is scattered across different hospitals. They may visit one center for diagnosis, another for surgery, and a third for chemotherapy or radiation therapy. This fragmented approach often results in: Delays in diagnosis Poor coordination between doctors Repeated tests and higher expenses Emotional stress for families “Under one roof” means a fully integrated cancer treatment center where diagnosis, treatment, supportive care, and follow-up happen in the same place. This structured model improves treatment accuracy, enhances survival rates, and ensures a smoother patient experience. A modern cancer treatment center in Mumbai offering integrated services allows patients to receive seamless care without losing valuable time. Comprehensive care ensures coordinated, timely, and precise cancer management. What Does “Comprehensive Oncology Care” Actually Mean? Comprehensive cancer care refers to complete, end-to-end cancer management. It covers every stage of the patient journey, including: Detection → Diagnosis → Staging → Treatment Planning → Active Treatment → Recovery → Follow-Up → Survivorship Unlike standalone facilities that provide only chemotherapy or surgery, a fully integrated oncology hospital offers multidisciplinary cancer care supported by advanced technology and expert coordination. Key Components of Complete Cancer Care Early cancer detection and screening Accurate cancer diagnosis and staging Personalized oncology treatment plans Advanced cancer treatment options Cancer supportive care Palliative cancer care Long-term cancer follow-up care Technology such as PET-CT scans, molecular testing, and genetic profiling improves diagnostic precision and allows doctors to monitor response continuously. Multidisciplinary Oncology Team: Backbone of Comprehensive Cancer Care Cancer is complex. One doctor alone cannot manage every aspect of diagnosis and treatment. That is why a cancer specialist’s team, also known as a tumor board, plays a critical role. During tumor board meetings, specialists review imaging reports, biopsy test results, staging details, and the patient’s overall health before finalizing the best cancer treatment plan. Specialists Involved in Multidisciplinary Cancer Care Medical Oncologist Manages chemotherapy, targeted therapy, immunotherapy, and hormone therapy. Monitors response and handles chemotherapy side effects. Surgical Oncologist Performs tumor removal surgeries, organ-preserving procedures, minimally invasive surgeries, and reconstructive cancer surgery. Radiation Oncologist Plans and delivers radiation therapy using precision techniques while protecting healthy tissues. Pathologist Confirms cancer diagnosis, determines tumor grading, and performs molecular testing. Radiologist Interprets CT scan, MRI, and PET-CT imaging to detect and monitor disease progression. Onco-nurses, Nutritionists, Psychologists, and Rehabilitation Experts Provide cancer supportive care, nutritional guidance, emotional counseling, and recovery support. This team-based approach ensures personalized and precise cancer patient care. Step-by-Step Oncology Care Under One Roof 1. Early Cancer Detection & Screening Early cancer detection significantly improves survival rates. Unfortunately, many patients ignore early cancer symptoms, such as: Persistent lumps Unexplained weight loss Continuous fatigue Abnormal bleeding Chronic cough Change in bowel habits Importance of Cancer Screening Regular cancer screening programs help detect cancer before symptoms appear. Common screening programs include: Breast cancer screening Cervical cancer screening Oral cancer screening Prostate cancer screening Colorectal cancer screening High-risk individuals, including those with family history or tobacco use, benefit greatly from routine screening. Benefits of Early Detection Less aggressive treatment Shorter recovery time Higher survival rates Reduced financial burden Better quality of life 2. Accurate Cancer Diagnosis & Staging An accurate cancer diagnosis forms the foundation of effective treatment. Diagnostic Process Includes the Following: Imaging Tests CT scan MRI PET-CT Biopsy Test Confirms cancer type Determines tumor characteristics Histopathology & Molecular Testing Identifies genetic mutations Guides targeted therapy Blood Tests & Tumor Markers Monitor disease progression Cancer Staging (Stage I–IV) Cancer staging determines how far the cancer has spread. Early-stage cancers may require surgery alone, while advanced stages may need combination therapy. Correct staging ensures the right personalized cancer treatment plan. 3. Personalized Cancer Treatment Planning Every patient is different. Personalized cancer treatment considers: Cancer type and stage Tumor biology Patient’s age and medical condition Genetic and molecular profile Patient preferences Doctors follow evidence-based clinical guidelines to design a customized oncology treatment plan. Continuous evaluation ensures treatment adjustments when necessary. Advanced Cancer Treatment Options Available Under One Roof A comprehensive oncology hospital provides all major cancer treatment options in one location. Medical Oncology Chemotherapy Destroys fast-growing cancer cells and prevents spread. Targeted Therapy Focuses on specific cancer-causing genetic mutations. Immunotherapy Strengthens the immune system to fight cancer. Hormone Therapy Used for hormone-sensitive cancers such as breast and prostate cancer. Surgical Oncology Tumor removal surgery Organ-preserving cancer surgeries Minimally invasive techniques Robotic-assisted surgery Reconstructive procedures Radiation Oncology External beam radiation therapy Intensity-Modulated Radiation Therapy (IMRT) Image-Guided Radiation Therapy (IGRT Combination therapies (surgery + chemotherapy + radiation therapy) often improve survival and long-term outcomes. Patients seeking oncology treatment in Mumbai benefit from access to these advanced technologies within an integrated oncology hospital. Supportive Care: Managing Side Effects & Improving Quality of Life Cancer treatment may cause: Fatigue Nausea Hair loss Pain Low immunity Emotional distress Cancer supportive care focuses on improving comfort and managing chemotherapy side effects through: Pain management programs Nutritional counseling Psychological therapy Infection control guidance Physical rehabilitation Holistic care improves treatment tolerance and quality of life. Palliative Care: Comfort, Dignity & Symptom Relief Palliative cancer care supports patients at any stage of illness. It is not limited to end-of-life situations. Services Include: Advanced pain management Symptom control Emotional and psychological support Family counseling Support during advanced cancer treatment Early integration of palliative care enhances comfort and dignity. Follow-Up Care & Cancer Survivorship After active treatment, structured cancer follow-up care is essential. Follow-Up Includes: Regular scans Blood tests Physical examinations Monitoring for recurrence Cancer Survivorship
- admin
- 0 Comments
Exercises After Knee Replacement: A Complete Guide for Faster Recovery
Taking care of yourself and being patient will help you heal after knee replacement surgery. The surgery will help with pain and movement, but the real success of the procedure depends on how well you stick to your recovery plan, especially the exercises you do after knee replacement. Our orthopedic specialists at Zynova Shalby Hospital always stress that physiotherapy and simple daily exercises are just as important as the surgery itself. These movements will help your knee get stronger, become more flexible, and make it easier for you to get back to your normal life. Why Are Exercises Important After Knee Replacement? A lot of people think that just resting after surgery is enough, but that’s not true. If you don’t do your exercises, your knee can get stiff and weak, which will make it take longer and hurt more to heal. Regular rehabilitation exercises after knee replacement are crucial because they: Make blood flow better and stop clots from forming. Make the joint less swollen and stiff. Strengthen the muscles around the knee to give it more support. Get back your balance and ability to walk. Make sure your new knee joint lasts a long time. When Can You Start Exercises After Knee Replacement? Most patients can start moving around gently within 24 hours of surgery with the help of a physiotherapist. As you get better, the routine gets better: Weeks 1–3: Exercises to improve flexibility and range of motion. Weeks 4–6: Practice walking and getting stronger. After six weeks: Activities that don’t put too much stress on your body to build endurance. Before starting or changing your exercise plan, always listen to what your doctor says. Best Exercises After Knee Replacement Here are some safe and effective exercises that our experts at Zynova Shalby Hospital often recommend: 1. Pumps for the Ankles : Put your back flat on the ground. Move your ankle up and down slowly, like you’re pressing and releasing a pedal. Do it again 10–15 times. Helps with swelling and better blood flow. 2. Sets for the quadriceps : Sit with your leg straight on the bed. Tighten your thigh muscles and push the back of your knee downwards. Hold for 5–10 seconds, then relax. Builds thigh strength and improves knee stability. 3. Heel Slides : Lie on your back with legs stretched. Slowly slide your heel toward your hip, bending the knee. Hold for a few seconds, then straighten the leg. Improves flexibility and bending ability. 4. Straight Leg Raises Lie down with the operated leg straight and the other bent. Lift the operated leg about 6–12 inches from the bed. Hold for 3–5 seconds, then lower slowly. Strengthens thigh and hip muscles without stressing the knee. 5. Knee Bends (Seated or Standing) Sit on a chair or stand with support. Bend your operated knee gently as far as it feels comfortable. Return slowly to the starting position. Strengthens thigh and hip muscles without stressing the knee. 6. Walking Begin with a walker or crutches. Take short, slow steps. Gradually increase your walking distance each day. Improves mobility, endurance, and overall confidence in using your new knee. Safety Tips While Doing Exercises While these exercises are safe, precautions are always important: If you experience severe pain, stop (some discomfort is normal). Steer clear of high-impact exercises like jumping and running. Exercise on a level, secure surface at all times. Utilize assistance as soon as possible. Never miss a follow-up appointment with your physiotherapist. Long-Term Exercises for Knee Health Once your recovery is complete, you can adopt low-impact exercises to keep your knee strong and flexible: Swimming – Gentle and effective without putting weight on the knee. Cycling – Builds strength and range of motion. Yoga and stretching – Enhances flexibility and balance. Light strength training – Keeps muscles strong for joint support. Conclusion Recovery from knee replacement surgery is a process that requires patience, and exercising is the most important step in the process. Exercising after knee replacement makes a person feel better, more comfortable, and confident to perform daily activities again. At Zynova Shalby Hospital in Ghatkopar, Mumbai, we feel that surgery is just half the process of recovery; complete rehabilitation is equally essential. Our experienced orthopedic surgeons and physiotherapy staff work closely with every patient to develop exercise programs that are both secure and efficient, promoting faster recovery and better long-term results. FAQs 1. When can I start exercises after knee replacement surgery? You can begin light exercises such as ankle pumps and thigh contractions within 24 hours after surgery, under the guidance of a physiotherapist. 2. What exercises should I avoid after knee replacement? Avoid high-impact activities like running, jumping, or heavy weightlifting, as they can strain your new knee joint. Stick to low-impact exercises recommended by your doctor. 3. Can I climb stairs after knee replacement surgery? Yes, but only after a few weeks and with proper guidance. Initially, use support and take one step at a time until your muscles are stronger.
- admin
- 0 Comments
Top 3 Most Common Types of Cancer in Women You Should Know
Introduction Did you know that cancer is one of the biggest health problems for women all over the world? But most of the time, it can be treated or stopped when it is found early. Sadly, most women don’t pay attention to the early signs because they think they’re just small health problems. The first step in protecting your health is to learn about the different kinds of cancer that can affect women. Being aware early on can literally mean the difference between life and death for people with breast cancer, cervical cancer, skin cancer, or ovarian cancer. Top 3 Most Common Types of Cancer in Women Cancer continues to pose a great danger to the health of women globally. Some of the most frequent forms of cancer in women include breast cancer, cervical cancer, and skin cancer. Let us get into detail about each of these forms of cancer in women, the signs they warn of, and why early diagnosis matters so much. Breast Cancer – It happens when breast cells divide and multiply too quickly and form a mass or tumor. The disease usually starts in the milk ducts or lobules, but if it isn’t treated, it can spread to other parts of the body. Breast cancer is the most common type of cancer in women around the world. The good news is that it can be found early if the patient does self-exams and mammograms on a regular basis. Warning Signs of Breast Cancer: A lump in the breast or underarm Alterations in the shape or the size of the breast Abnormal nipple discharge Skin dimpling or redness on the breast Why Early Detection of Breast Cancer is Vital: Breast cancer boasts one of the best survival rates if found early. Screening mammograms and regular self-examinations are lifesavers that identify abnormalities early, when they are not yet able to metastasize. Tips For Preventing Breast Cancer: Have a healthy weight and be physically active Reduce alcohol intake Breastfeed if possible Pay attention to your family’s health history Cervical Cancer – The cervix, the lower part of the uterus near the vagina, is where cervical cancer starts. Persistent human papillomavirus (HPV) infection is the main cause. Routine Pap smears and HPV testing detect it even before it manifests as cancer because it typically starts as precancerous abnormalities. Warning Signs of Cervical Cancer: Abnormal bleeding (perimenstrual, after intercourse, or after menopause) Abnormal vaginal discharge Pain during intercourse or pelvic discomfort Why Screening Matters for Cervical Cancer: Most cervical cancers arise because women do not attend routine Pap smears or HPV tests. Early detection of precancerous characteristics greatly improves the success of treatment. How to Prevent Cervical Cancer: Get the HPV vaccine. HPV infection is the main cause of cervical cancer, so getting the vaccine can greatly lower your risk. Regular Pap Smears and HPV Testing: Pap smears can find changes in the cervix that aren’t normal before they turn into cancer, and HPV testing can find infections early. When you’re intimate, be safe. Using protection can help lower your risk of getting HPV. Stop smoking. Smoking weakens the immune system, which makes it harder for the body to fight HPV infections. Cervical cancer is different because it can be found before it becomes cancer, which makes it very easy to stop. Women should never miss their regular screenings because the best way to protect themselves is to find problems early. Skin Cancer in Women Another of the most prevalent cancers in women is skin cancer, which is mostly brought on by exposure to ultraviolet (UV) radiation from tanning beds or the sun. Skin cancer can strike anyone, but it is more likely to strike women who spend a lot of time outside without protection. Melanoma is the most aggressive of its types, whereas squamous and basal cell carcinomas are more prevalent but less difficult to treat. Warning Signs of Skin Cancer New moles or growths that change in shape, size, or color Sores or wounds that persist Rough, red, or scaly skin patches Itching, bleeding, or mole pain One helpful method for spotting melanoma is the ABCDE rule: A – Asymmetry: The mole’s two halves are not identical Border: Uneven or hazy edges Color: Various tones of red, black, or brown Diameter: More than 6 mm Evolving: Any change in size, color, or shape Importance of Early Detection and Regular Screenings The most important thing that connects breast cancer, cervical cancer, and skin cancer is the fact that all of them can often be detected early. Regular screenings, health check-ups, and self-examinations allow women to identify unusual changes in their bodies before they turn into serious problems. Preventive healthcare should never be ignored, as early intervention improves survival rates significantly. Women must also be aware of their family medical history, lifestyle factors, and environmental risks. For example, if breast cancer runs in your family, mammograms may need to start earlier than the general recommendation. Similarly, if you are frequently exposed to the sun, protecting your skin should be a daily habit. General Tips to Reduce Cancer Risk in Women You can’t stop all cancers, but you can lower your risk a lot by making smart choices about your health: Eat a balanced diet that includes whole grains, fruits, vegetables, and lean proteins. Stay active: You should work out for at least 30 minutes most days of the week. Don’t smoke and drink only in moderation. Use sunscreen and stay away from tanning beds to protect your skin from the sun. Get your shots: One of the best ways to avoid cervical cancer is to get the HPV vaccine. Get regular checkups and screenings for your health. Conclusion Cancer is a word that can cause fear, but knowledge and early detection can save lives. The top 3 most common types of cancer in women – breast cancer, cervical cancer, and skin cancer – can often be prevented or successfully treated if identified early. By paying attention to warning signs,
- admin
- 0 Comments
Heart Bypass Surgery Recovery Time: Essential Tips for a Faster and Smoother Recovery
Introduction Heart bypass surgery, which is also known by coronary artery bypass grafting (CABG), is a highly common surgery that is performed to restore blood flow into the heart when the arteries are blocked or narrowed. Even though surgery itself is a milestone, patients and their families are equally concerned about what happens after the recovery period. Education on recovery time after bypass surgery on the heart, precautions, and what one can expect during each stage of recovery is key in ensuring a problem-free and safe recovery. At Zynova Shalby Hospital, patient education is highly valued, and an educated patient recovers better. This blog is intended to guide you through each stage of recovery after bypass surgery, timeline, advice on care, limitations, and when to watch out for medical attention. What is Bypass Surgery Bypass surgery, or coronary artery bypass grafting (CABG), is a surgical procedure intended to improve blood flow into the heart. It is usually recommended for people who have severe coronary artery disease, where the coronary arteries that feed blood into the heart are blocked or narrowed by plaque buildup. During surgery, doctors take a healthy blood vessel from another part of the body—most often the leg, arm, or chest—and attach it to the heart. This new vessel creates a “bypass” around the blocked artery, ensuring oxygen-rich blood can continue flowing to the heart muscle. The procedure is highly effective in easing chest pain (angina), improving stamina, and lowering the risk of a heart attack in patients with significant blockages. It is generally suggested when lifestyle changes, medication, or less invasive procedures like angioplasty are not enough to restore circulation. How Long is the Recovery Time After Bypass Surgery? Recovery after bypass surgery happens gradually and can differ for each person depending on their age, overall health, lifestyle, and the number of grafts done. On average: Hospitalization: Most patients remain in the hospital for about 5–7 days after surgery. Early Recovery (First 6–8 Weeks): This stage focuses on regaining mobility, strength, and independence. Full Recovery: It may take around 3–6 months for the body to completely heal and for energy levels to return to normal. Remember, recovery does not only mean physical healing but also regaining emotional strength and confidence. What to Expect in First Weeks In the early days, patients may notice: Chest discomfort after bypass surgery due to healing of the breastbone. Swelling or soreness at the incision site or in the leg (if veins were taken from there). Tiredness and low energy as the body focuses on recovery. Mood changes or anxiety, which are normal after major surgery. It’s important not to panic if you feel chest pain after bypass surgery, as mild discomfort is part of the healing process. However, severe or persistent pain should always be reported to your doctor. Essential tips for faster recovery of Bypass Surgery Follow Medical Advice Strictly Your healthcare team will provide specific instructions about medications, wound care, and lifestyle changes. Taking your prescribed medicines on time helps prevent complications like infections, blood clots, or irregular heartbeat. Pay Attention to Wound Care Incision care is one of the most important aspects of after bypass surgery care. Keep the surgical site clean and dry. Watch out for signs of infection such as redness, swelling, or unusual discharge. Manage Pain Effectively It’s natural to have some chest discomfort after bypass surgery. Taking prescribed painkillers and practising relaxation techniques can make recovery easier. Avoid over-the-counter medication unless your doctor approves. Gradual Physical Activity Walking is the best form of exercise during the recovery phase. Begin with short walks and slowly increase duration and intensity as advised. Physical therapy or a cardiac rehabilitation program plays a big role in rebuilding strength and stamina. 5. Monitor Your Diet Carefully A heart-healthy diet is vital for recovery and long-term well-being. Include fresh fruits, vegetables, whole grains, lean proteins, and healthy fats. Reduce salt, sugar, and saturated fats to support heart function and prevent future blockages. 6. Sleep and Rest Well Adequate rest speeds up bypass surgery recovery time. Sleep may be challenging initially due to discomfort, but using pillows for support and practicing relaxation before bedtime can help. 7. Emotional Healing Matters It’s common to feel low or anxious after heart surgery. Joining support groups, practicing meditation, or counseling can help patients cope better with post-surgery emotional stress. Precautions after bypass surgery Taking the right *precautions after bypass surgery* ensures long-term benefits and prevents setbacks: Avoid Heavy Lifting: Refrain from lifting anything heavier than 2–3 kg for the first few weeks. No Driving Initially: Patients should avoid driving for at least 4–6 weeks or until cleared by their doctor. Careful with Stairs: Use support when climbing stairs in the early stages. Avoid Smoking & Alcohol: Both can slow recovery and increase the risk of complications. Regular Monitoring: Keep track of blood pressure, blood sugar, and cholesterol levels. Lifestyle Changes for Long-Term Recovery Bypass surgery not only saves lives but also offers a second chance to build a healthier lifestyle. Here are a few long-term habits to adopt: Regular exercise (walking, cycling, yoga as permitted). Stress management through meditation or breathing exercises. Heart-friendly diet low in cholesterol and trans fats. Regular medical checkups and adherence to prescribed medications. Conclusion Heart bypass surgery is a major milestone, but recovery can be smooth and successful with the right care and guidance. While every patient’s healing journey is unique, following precautions, recognizing early warning signs, and making necessary lifestyle changes are key to regaining strength and returning to an active life. At Zynova Shalby Hospital, Ghatkopar, our team of expert cardiologists and cardiac surgeons go beyond surgery—we walk with you through every stage of recovery. With advanced technology, personalized rehabilitation, and compassionate care, we are dedicated to helping you and your loved ones live healthier, stronger, and longer lives. If you or someone close to you is preparing for bypass surgery, choose Zynova Shalby Hospital for trusted expertise, complete heart care, and a recovery journey you
- admin
- 0 Comments
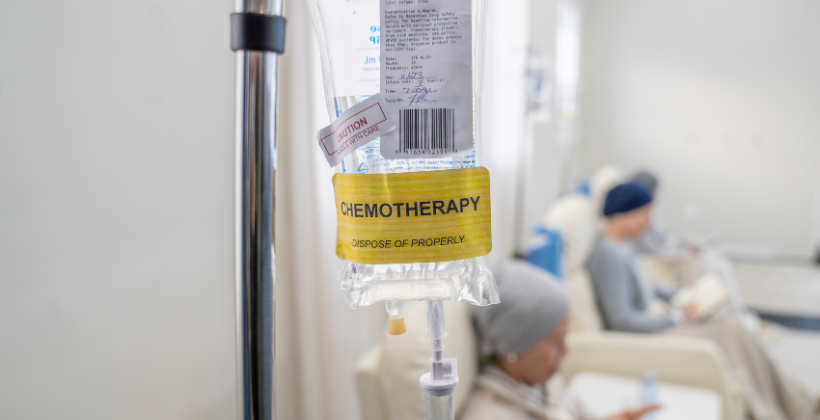
Chemotherapy for Blood Cancer: Understanding Treatment Options, Benefits, and What to Expect
Introduction Getting a diagnosis of blood cancer can change your life, but it’s important to remember that there is real hope with today’s advanced treatments. Chemotherapy for blood cancer is one of the most powerful and widely used treatments. It is very important for killing off abnormal blood cells and improving survival rates. Chemotherapy is often the first thing doctors do to stop leukemia, lymphoma, or multiple myeloma from spreading and get patients ready for other treatments like stem cell transplant. But what does chemotherapy really mean? How long does it take? What are the side effects, and how can you deal with them? This blog will tell you everything you need to know about chemotherapy for blood cancer, such as the different types of treatment available, their pros and cons, and what to expect before, during, and after therapy. The first step to getting better is to understand your treatment journey. We are here to help you every step of the way. What is Blood Cancer and How Does Chemotherapy Help? Blood cancer starts in the bone marrow, blood, or lymphatic system. Blood cancer changes how blood cells are made and how they work, unlike solid tumors. Leukemia affects white blood cells, lymphoma affects the lymphatic system, and multiple myeloma affects plasma cells. These are the three main types. These cancers make it harder for the body to fight infections, move oxygen around, and stop bleeding. Chemotherapy is a major treatment for blood cancer that uses strong anti-cancer drugs to kill blood cells that are growing too quickly. Chemotherapy is usually given systemically, either through oral pills or IV infusions, so it can reach all of the cells in the body that are affected by blood cancer. It helps shrink cancer, bring it into remission, and get the patient ready for a stem cell transplant in many cases. Chemotherapy has a good chance of controlling and curing the disease, especially if it starts early and is done by a professional. It does this by targeting abnormal cells in the blood and bone marrow. Types of Chemotherapy Used in Blood Cancer Chemotherapy for blood cancer isn’t a one-size-fits-all solution. It’s typically administered in carefully structured phases to enhance its effectiveness while reducing the risk of relapse. The treatment plan can differ based on the specific type of blood cancer—like leukemia, lymphoma, or myeloma—as well as factors such as the patient’s age, overall health, and how they respond to the treatment. Here are the main types of chemotherapy protocols that are commonly used: Induction therapy – Induction therapy marks the beginning and most intense stage of chemotherapy for blood cancer. The primary aim here is to swiftly eliminate as many cancer cells as possible and achieve remission. This approach is commonly used for acute leukemia and usually necessitates hospitalization because of the powerful combinations of drugs involved. Consolidation Therapy – Consolidation chemotherapy is meant to get rid of any cancer cells that may still be present but weren’t visible or detectable after the first induction therapy. These cells could cause a relapse. This stage is very important for keeping the remission going. Depending on how well the patient responded, consolidation therapy may use the same chemotherapy drugs as the induction phase or a different set of drugs. The goal is to lower the risk of relapse even more by using high-dose chemotherapy or chemotherapy with other treatments, such as stem cell transplants. Maintenance Therapy: – Taking care of Chemotherapy is usually given for a longer time after induction and consolidation to help keep the cancer from coming back and lower the risk of it coming back. During this phase, the goal is to keep cancer cells from spreading while the patient heals. It usually uses lower doses of chemotherapy drugs and can be given in cycles for months or even years, depending on the type of cancer and the patient’s health. This treatment helps keep any cancer cells that are still there under control. Combination Chemotherapy: – Combination chemotherapy is used to treat a lot of blood cancers, especially leukemia and lymphoma. This means using more than one chemotherapy drug, usually from different classes, that work together to attack different parts of the cancer cell’s life cycle. For instance, in lymphoma, drugs like cyclophosphamide and doxorubicin are used together to attack cancer cells at different points in their growth. Combination therapies are especially helpful for blood cancers because these diseases are so complicated and can become resistant to treatments that only use one drug. Intrathecal Chemotherapy – In some blood cancers, like leukemia, cancer cells can move to the brain or spinal cord. For these kinds of problems, intrathecal chemotherapy is used. This treatment involves putting chemotherapy drugs directly into the cerebrospinal fluid through a lumbar puncture. It helps to find cancer cells in the central nervous system and stop them from spreading. People often use this method with systemic chemotherapy to make sure that cancer cells are killed in every part of the body. Benefits of Chemotherapy Chemotherapy is still one of the best and most common ways to treat different kinds of blood cancer, like leukemia, lymphoma, and multiple myeloma. Chemotherapy for blood cancer has many important benefits that help with recovery and long-term remission when it is given by a qualified hemato-oncologist. This is how it helps: Aims at and kills cancer cells In a systematic way – Chemotherapy works against blood cancers that spread throughout the body because it goes through the bloodstream. This is different from surgeries or localized treatments. It goes after cancer cells wherever they are, but it is most effective in the bone marrow, where abnormal blood cells start to grow. Helps get into remission – Chemotherapy often works to put blood cancer into remission, especially when it is still in its early stages. It cuts down on the number of cancerous cells by a lot, which gives the patient a better chance of living longer and getting better. Gets the body
- 1
- 2